Inflammatory Back Pain
Almost all of us experience low back pain at some point in our lives. For many people, it’s related to common mechanical causes such as muscle strain, osteoarthritis (often described as “wear and tear”), bulging or herniated discs, or pinched nerves. This type of back pain can of course be uncomfortable and disruptive, but in many cases it improves with conservative treatments like physical therapy, stretching, activity modification, and time.
However, not all back pain is the same.
In some individuals, low back pain can be a sign of an underlying inflammatory or autoimmune condition. This type of pain is called inflammatory back pain, and recognizing it early is important because it is treatable. Unfortunately, inflammatory back pain is often overlooked or misattributed to mechanical causes, leading to years of unnecessary suffering.
As a rheumatologist, I see this scenario frequently. Patients come in after years of being told their pain is “normal,” “just aging,” or something they need to push through. Once we look more closely, the pattern of symptoms sometimes tell us something different.
Common Causes of Low Back Pain
Most low back pain is mechanical in nature.
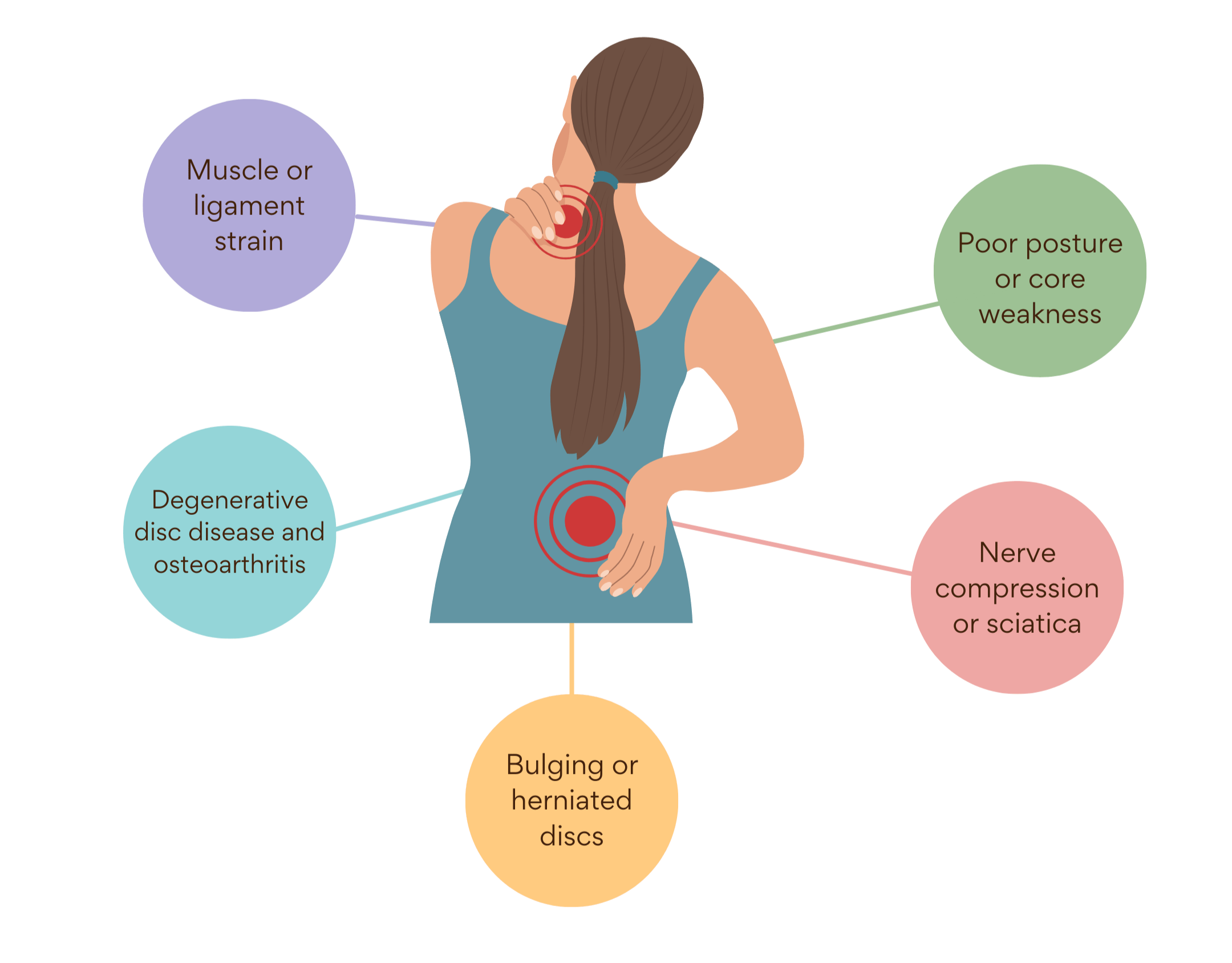
Common causes of back pain include:
Muscle or ligament strain
Degenerative disc disease and osteoarthritis
Bulging or herniated discs
Nerve compressions or sciatica
Poor posture or core weakness
Mechanical back pain often:
Worsens with activity
Improves with rest
Is triggered by a specific movement or injury
Feels predictable with certain positions
With appropriate conservative care, mechanical back pain often improves or resolves over time.
Inflammatory back pain behaves very differently.
What Is Inflammatory Back Pain?
Inflammatory back pain is caused by inflammation in the joints of the spine and pelvis, particularly the sacroiliac (SI) joints. It is commonly associated with rheumatologic and autoimmune conditions such as:
Ankylosing spondylitis (AS)
Axial spondyloarthritis (including non-radiographic disease)
Psoriatic arthritis
Inflammatory bowel disease–associated arthritis
These conditions are driven by immune system dysregulation and cause chronic inflammation that can affect much more than just the spine.
6 Key Features of Inflammatory Back Pain
1. Pain That Is Worse With Rest and Better With Movement
One of the most important clues is how the pain behaves throughout the day.
Inflammatory back pain tends to be worse after prolonged rest, such as:
Sitting on the couch watching a movie
Long car rides
Sleeping overnight
People often describe feeling their worst when they first get up, with significant stiffness and pain. Movement, walking, stretching, or gentle activity tends to improve symptoms, which is the opposite of mechanical back pain.
If your back feels stiff and painful when you stop moving, but loosens up as you get going, that is a classic inflammatory pattern.
2. Prolonged Morning Stiffness
With inflammatory back pain, stiffness:
Occurs almost every morning
Lasts 30 minutes to over an hour
Improves gradually with movement
Occasional morning stiffness can happen with many conditions, but persistent, prolonged stiffness is a red flag for inflammatory disease.
3. Pain that wakes you up at night
Back or buttock pain that regularly wakes you from sleep is not typical mechanical pain.
Many patients with inflammatory back pain describe waking up in the early morning hours with deep pain or stiffness and needing to get up and move around to feel better. This is a particularly important symptom that should prompt further evaluation.
4. Buttock (Gluteal) Pain
Inflammatory back pain often involves the SI joints, which can cause:
Deep buttock pain
Pain that alternates from one side to the other
Pain that doesn’t feel like a typical muscle strain
This pain is often mistaken for sciatica or a muscular issue, but its pattern and persistence can suggest inflammation.
5. Significant Fatigue
Inflammatory and autoimmune diseases can cause profound fatigue that goes beyond normal tiredness.
Patients often describe feeling:
Drained or heavy
Exhausted despite adequate sleep
Unable to recover energy easily
When back pain is paired with this kind of fatigue, it raises concern for a systemic inflammatory condition.
6. Onset at a Younger Age
Inflammatory back pain often begins in the early 20s to 40s, which is younger than typical degenerative back pain.
If someone develops persistent back pain with inflammatory features at a younger age, this should not be dismissed as “normal aging.”
Why Is It Important to identify Inflammatory Back Pain?
One of the most important things I want patients to know is this:
You do not have to suffer. You do not have to just power through chronic pain.
Inflammatory back pain is treatable, and effective therapies can significantly improve pain, stiffness, fatigue, and quality of life. Early diagnosis and treatment matter because untreated chronic inflammation can lead to:
Progressive joint damage
Loss of spinal mobility
Chronic pain and stiffness
Ongoing fatigue
Negative effects on overall health
Chronic systemic inflammation is not good for the body, and addressing it early leads to better long-term outcomes.
Why Does Early Diagnosis Matter?
In my practice, I’ve diagnosed inflammatory conditions in patients whose symptoms were initially subtle. In some cases, mild skin findings combined with back pain and fatigue led to a diagnosis of psoriatic arthritis. In others, imaging confirmed ankylosing spondylitis or related conditions.
Once treatment was started, many of these patients experienced meaningful improvement in pain, stiffness, fatigue, and daily functioning.
What Are Treatment Options for Inflammatory Back Pain?
Treatment depends on the specific diagnosis and individual circumstances but may include:
Anti-inflammatory medications
Physical therapy and targeted exercise
Disease-modifying medications, including biologic therapies such as Adalimumab (Humira)
Lifestyle strategies to support overall health and inflammation control
The goal is not only symptom relief, but controlling inflammation and protecting long-term health.
Key Takeaways
• Pain that is worse with rest and improves with movement
• Morning stiffness lasting more than 30 minutes
• Back or buttock pain that wakes you from sleep
• Significant, ongoing fatigue
• Symptoms beginning in your early 20s to 40s
• A personal or family history of autoimmune disease
Know your body
Persistent symptoms deserve careful evaluation and early diagnosis leads to better health outcomes.