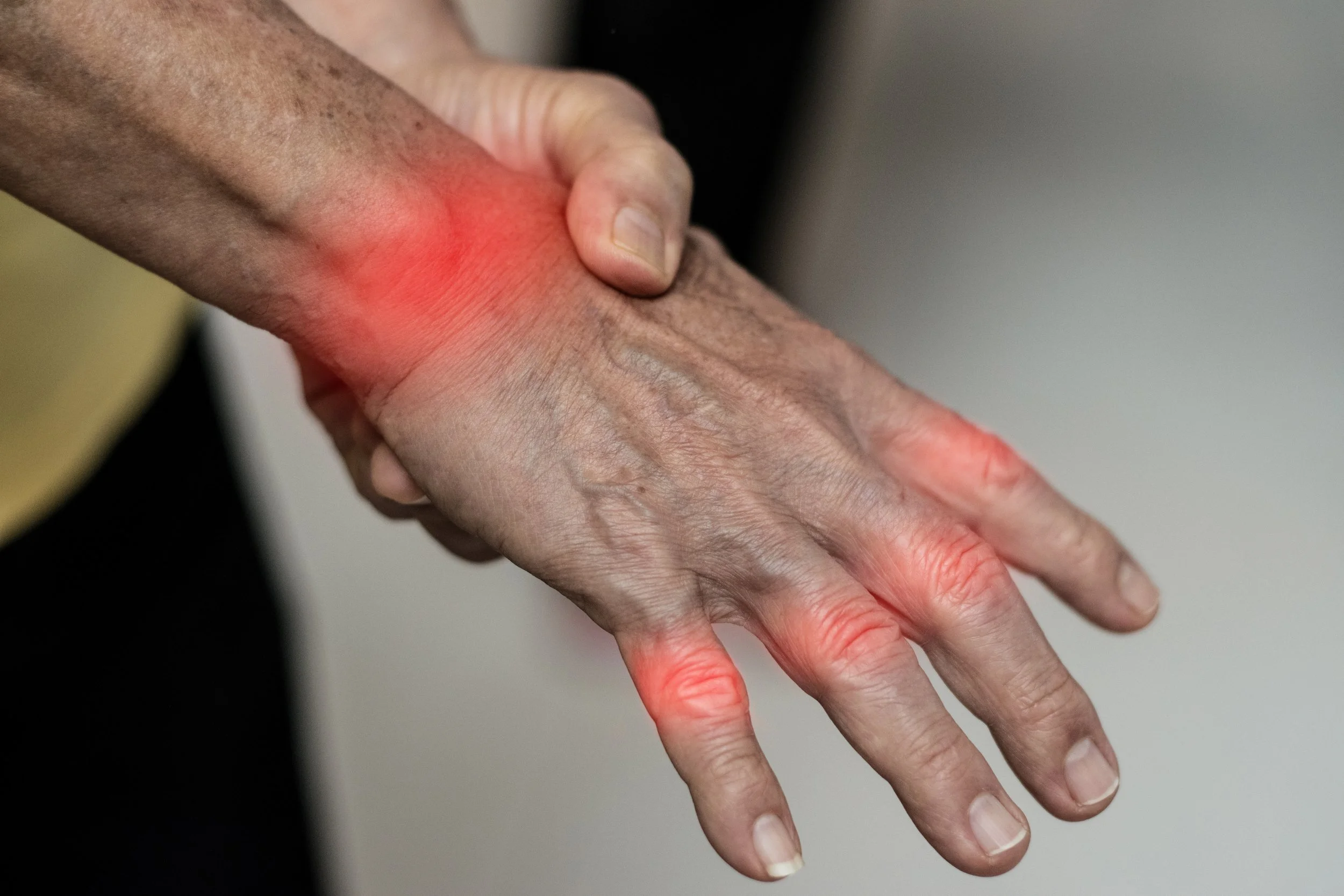
Psoriatic Arthritis: More Than Just Skin Disease
When most people hear “psoriasis,” they think of a skin condition. But psoriatic arthritis (PsA) is far more than that—it’s a complex inflammatory disease that can affect your joints, nails, and even where tendons attach to bone (called entheses). Recognizing these symptoms early can make a meaningful difference in long-term outcomes.
“My skin isn’t that bad—could I still have psoriatic arthritis?”
Yes. Joint symptoms don’t always match the severity of skin disease. Some patients have minimal or even no visible psoriasis when joint pain begins. If you have a personal or family history of psoriasis and develop joint pain, stiffness, or swelling, it’s worth evaluating.
“What kind of joint symptoms should I look for?”
PsA can affect joints in different patterns. You may notice:
Swelling in entire fingers or toes (“sausage digits”)
Morning stiffness lasting more than 60 minutes
Pain that improves with movement rather than rest
Asymmetric joint involvement (not the same joints on both sides)
“Why are my nails changing?”
Nail changes are a key clue. Pitting (tiny dents), separation from the nail bed, or thickening may signal underlying inflammation. Nail disease is closely linked with joint involvement, especially in the fingers.
“What is enthesitis—and why does my heel hurt?”
Enthesitis is inflammation where tendons and ligaments attach to bone. Common areas include:
Heels (Achilles tendon or plantar fascia)
Elbows
Knees
This pain can feel different from joint pain—more localized, often worse with activity or pressure.
Practical Takeaways
Don’t ignore joint pain just because your skin symptoms seem mild.
Take photos of swelling or rashes—symptoms can fluctuate.
Mention nail changes to your doctor—they are clinically meaningful.
Early treatment can prevent joint damage and improve quality of life.
Tips
Track your symptoms: note stiffness duration, swelling, and triggers.
Stay active: gentle movement can reduce stiffness and maintain function.
Advocate for yourself: if something feels off, ask for a rheumatology evaluation.
Understand your options: treatments today are highly effective and the science has advanced so much with regards to treatments for PsA.
Psoriatic arthritis is a systemic condition—not just skin deep. The earlier it’s recognized, the more we can do to protect your joints, function, and long-term health.
Additional references:
Kharouf F, Gladman DD. "Advances in theManagement of Psoriatic Arthritis inAdults" BMJ. 2024
This comprehensive yet accessible review published in BMJ covers the full spectrum of PsA management.
https://www.bmj.com/content/387/bmj-2024-081860.long
Kannappan R, Kim S, Lau A, Brent LH. "Psoriatic Arthritis: From Diagnosis to Treatment" Journal of Clinical Medicine. 2025
This very recent comprehensive review provides an integrated approach from diagnosis through treatment.